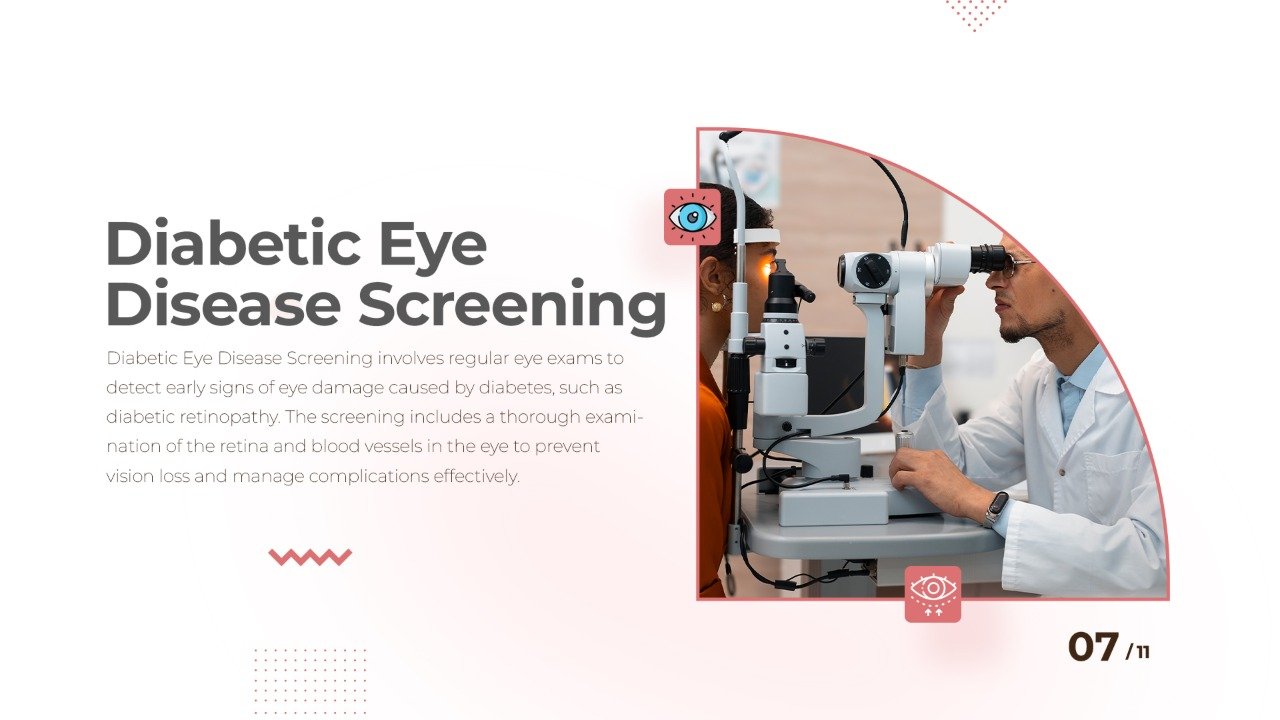

How Diabetes Affects Your Eyes
Diabetes is one of the leading causes of preventable blindness in adults globally, and India bears a disproportionately high burden of this disease. Prolonged high blood sugar levels damage the small blood vessels that supply the retina — the light-sensitive tissue at the back of the eye — causing a condition known as diabetic retinopathy. This damage can progress without any noticeable change in vision, making regular screening the only reliable way to detect it before irreversible harm occurs.
In addition to diabetic retinopathy, people with diabetes are at higher risk of developing diabetic macular oedema (swelling at the centre of the retina), early-onset cataracts, and a greater susceptibility to glaucoma. Each of these conditions requires different management and underscores the importance of comprehensive, regular eye care for every patient living with diabetes.
Who Needs Diabetic Eye Screening?
All patients with type 1 or type 2 diabetes should undergo a comprehensive dilated eye examination at least once a year — regardless of how long they have had diabetes or how well their blood sugar is currently controlled. Diabetic eye disease can develop even when glucose levels appear to be reasonably managed. Women with diabetes who become pregnant require more frequent screening, as pregnancy can accelerate retinal changes.


What Diabetic Eye Screening Involves
At our clinic in Malad, Dr. Archana Sanghvi Gotecha performs dedicated diabetic eye disease screening as part of a comprehensive dilated examination. The evaluation looks for:
Signs of haemorrhage, exudates, or abnormal blood vessel growth in the retina

Macular involvement — changes at the centre of the retina affecting sharp, detailed vision

Intraocular pressure measurement to screen for associated glaucoma

Lens assessment to detect diabetes-related cataract changes
Stages of Diabetic Retinopathy
Diabetic retinopathy is classified from mild non-proliferative disease — where small changes are present in the retinal vessels — to severe proliferative retinopathy, where fragile new blood vessels grow and carry a high risk of haemorrhage and retinal detachment. Early detection at the mild stage allows for intervention or closer monitoring that can prevent progression to the more damaging stages.
Treatment & Coordinated Care
Management depends on the stage and severity of diabetic eye disease. Mild cases may require only more frequent monitoring and optimisation of diabetes, blood pressure, and cholesterol control. Advanced stages may require laser therapy, intravitreal injections, or in some cases surgical evaluation. Dr. Gotecha coordinates closely with patients’ diabetologists and physicians to ensure a holistic approach that addresses both the eye and the systemic disease.
Stages of Diabetic Retinopathy
Mumbai’s urban population faces significant diabetes risk due to lifestyle factors — irregular dietary habits, physically sedentary roles, high stress, and disrupted sleep patterns. Raising awareness about annual diabetic eye screening within this population is a public health priority that Dr. Gotecha actively supports through patient education at every consultation.
Frequently Asked Questions
A: All patients with diabetes are advised to have a comprehensive dilated eye examination at least once a year. Those with existing diabetic retinopathy or other ocular complications may require more frequent monitoring as advised by their ophthalmologist.
A: Early-stage diabetic retinopathy can often be stabilised with good metabolic control — blood sugar, blood pressure, and cholesterol management. However, structural damage caused by advanced disease cannot be fully reversed. Treatment at the appropriate stage can slow or halt further progression, which is why early detection through regular screening is so important.
